JAKAFI® or JAKAFI XR™ (ruxolitinib) is a prescription medication used to treat adults with certain types of myelofibrosis (MF). It is not known if JAKAFI or JAKAFI XR is safe or effective in children for treatment of myelofibrosis.
Hear from real patients who share their unique perspectives on their myelofibrosis (MF) journey with Jakafi® (ruxolitinib). Individual results may vary.

I’m doing pretty darn good.
When Suzanne gave birth to her son in 1993, her joy came with unexpected news: She had a rare, chronic blood cancer called essential thrombocythemia (ET). Soon after her diagnosis, Suzanne partnered with a local hematologist to help manage her condition. Her ET was well controlled for nearly 10 years until her disease—along with her
symptoms—began to change.
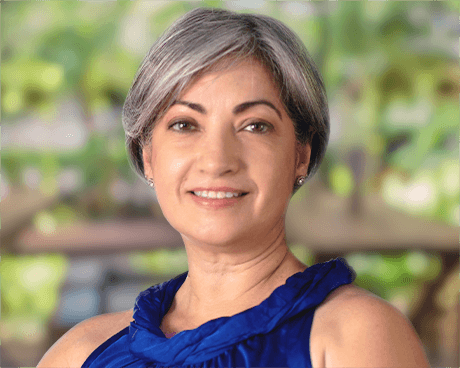
I was really scared when I was diagnosed.
Having been a graphic designer for most of her life, Mayra was used to exploring creative solutions. However, when she turned 50 and started to experience severe night sweats, there didn’t seem to be anything designed to help her escape them. Knowing that night sweats were a common symptom of premenopause, she assumed that
JAKAFI or JAKAFI XR (ruxolitinib) is a prescription medication used to treat adults with certain types of myelofibrosis (MF).
It is not known if JAKAFI or JAKAFI XR is safe or effective in children for treatment of myelofibrosis.
JAKAFI or JAKAFI XR is a prescription medication used to treat adults with polycythemia vera (PV) who have already taken a medicine called hydroxyurea and it did not work well enough or they could not tolerate it.
It is not known if JAKAFI or JAKAFI XR is safe or effective in children for treatment of polycythemia vera.
JAKAFI or JAKAFI XR is a prescription medication used to treat adults and children 12 years of age and older with acute graft-versus-host disease (GVHD) who have taken corticosteroids and they did not work well enough.
JAKAFI or JAKAFI XR is a prescription medication used to treat adults and children 12 years of age and older with chronic graft-versus-host disease (GVHD) who have taken one or two types of treatments and they did not work well enough.
JAKAFI or JAKAFI XR can cause serious side effects, including:
Low blood counts: JAKAFI or JAKAFI XR may cause low platelet, red blood cell, and white blood cell counts. If you develop bleeding, stop taking JAKAFI or JAKAFI XR and call your healthcare provider. Your healthcare provider will do a blood test to check your blood counts before you start and regularly during your treatment. Your healthcare provider may change your dose or stop your treatment based on the results of your blood tests.
Tell your healthcare provider right away if you develop or have worsening symptoms such as
Infection: You may be at risk for developing a serious infection during treatment with JAKAFI or JAKAFI XR. Tell your healthcare provider if you develop any of the following symptoms of infection:
Worsening of symptoms after interrupting or stopping treatment. Signs and symptoms of myelofibrosis may worsen after you stop treatment.
Do not interrupt or stop treatment without talking to your healthcare provider. Tell your healthcare provider right away if you have any of the following after stopping treatment:
Cancer: Some people have had certain types of non-melanoma skin cancers during treatment with JAKAFI or JAKAFI XR. Your healthcare provider will regularly check your skin during your treatment. Tell your healthcare provider if you develop any new or changing skin lesions during treatment.
Increases in cholesterol: You may have changes in your blood cholesterol levels during treatment with JAKAFI or JAKAFI XR. Your healthcare provider will do blood tests to check your cholesterol levels about every 8 to 12 weeks after you start taking JAKAFI or JAKAFI XR and as needed.
Increased risk of major cardiovascular events such as heart attack, stroke or death in people who have cardiovascular risk factors and who are current or past smokers while using another JAK inhibitor to treat rheumatoid arthritis:
Get emergency help right away if you get any symptoms of a heart attack or stroke during treatment with JAKAFI or JAKAFI XR, including:
Increased risk of blood clots: Blood clots in the veins of your legs (deep vein thrombosis, DVT) or lungs (pulmonary embolism, PE) have happened in people taking another JAK inhibitor for rheumatoid arthritis and may be life-threatening.
Tell your healthcare provider right away if you have any signs and symptoms of blood clots during treatment with JAKAFI or JAKAFI XR, including:
Possible increased risk of new (secondary) cancers: People who take another JAK inhibitor for rheumatoid arthritis have an increased risk of new (secondary) cancers, including lymphoma and other cancers. People who smoke or who smoked in the past have an added risk of new cancers.
The most common side effects of JAKAFI or JAKAFI XR include:
These are not all the possible side effects. Ask your pharmacist or healthcare provider for more information. Call your doctor for medical advice about side effects.
Before taking JAKAFI or JAKAFI XR, tell your healthcare provider about:
Women should not take JAKAFI or JAKAFI XR while pregnant or planning to become pregnant. Do not breastfeed during treatment with JAKAFI or JAKAFI XR and for 2 weeks after the final dose.
How should I take JAKAFI or JAKAFI XR?
Please see the Full Prescribing Information, including Patient Information, which includes a more complete discussion of the risks associated with JAKAFI or JAKAFI XR.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch, or call 1-800-FDA-1088.
You may also report side effects to Incyte Medical Information at 1-855-463-3463.