Possible Benefits of Jakafi®
The REACH3 Clinical Study with Jakafi
To better understand how medicines work and what side effects they may cause, researchers perform clinical trials in which patients with a particular condition receive a medicine and researchers observe the results.
Jakafi® (ruxolitinib) was studied in a clinical trial, called the REACH3 study, in patients with chronic graft-versus-host disease (GVHD) who have already taken corticosteroids and they did not work well enough.
Who was included in the REACH3 study of Jakafi for chronic GVHD?
A total of 329 patients with chronic GVHD who were not responding well to steroids, with or without other medicines that suppress the immune system, were enrolled in this clinical trial.
Half (165 patients) were treated with Jakafi; the other half (164 patients) were treated with one or more of a limited group of other treatments that are commonly used for chronic GVHD.
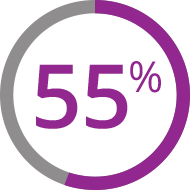
About 55% (180 of 329 patients in this study) had previous acute GVHD.
What else should I know about patients in the study?
Patients in the two treatment groups were similar in terms of disease severity and age.
In the Jakafi group: 48% (79 of 165) had moderate and 52% (86 of 165) had severe chronic GVHD. In the other treatments group: 52% (85 of 164) had moderate and 48% (79 of 164) had severe chronic GVHD. Overall, patients ranged in age from 12 to 76 years; average age of 49 years in the Jakafi group and 50 years in the other treatments group.
How was response to treatment measured and defined?
The main goal of this study was to assess each patient for their:
- Overall response to treatment: which meant either a:
- Complete resolution of all original signs and symptoms of chronic GVHD (complete response)
- or
- At least some improvement in at least one affected area without worsening signs or symptoms in other areas (partial response)
Researchers also assessed for:
- Symptom improvement: which meant at least a 7-point reduction in patient-reported symptoms at any point through the 24 weeks compared with the start of the study based on a standardized rating scale of 0 to 100 (no symptoms to worst symptoms)
Possible benefits of Jakafi when studied against other therapies for chronic GVHD
More patients treated with Jakafi experienced a response compared with
patients who were treated with other therapies
At 24 weeks:
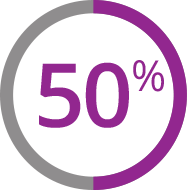
(82 of 165 patients)
treated with Jakafi
VS
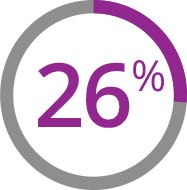
(42 of 164 patients)
treated with other study therapies
At any point through the 24 weeks:
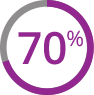
(116 of 165 patients)
treated with Jakafi
VS
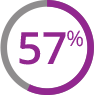
(94 of 164 patients)
treated with other study therapies
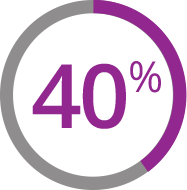
40% (66 of 165) of patients treated with Jakafi reported symptom reduction at any point through the 24 weeks

Your results with Jakafi may vary. Talk to your Transplant Team about any questions you have and whether jakafi is right for you.

Already taking Jakafi? IncyteCARES for Jakafi is a patient support program helping eligible patients with access and support.
Learn More
Chronic GVHD can affect many parts of the body.
Be sure to watch for any new or worsening signs and symptoms and discuss them with your Transplant Team right away.
Review SymptomsINDICATIONS AND USAGE
INDICATIONS AND USAGE
Jakafi is a prescription medicine used to treat adults with polycythemia vera who have already taken a medicine called hydroxyurea and it did not work well enough or they could not tolerate it.
Jakafi is used to treat adults with certain types of myelofibrosis.
Jakafi is used to treat adults and children 12 years of age and older with acute graft-versus-host disease (GVHD) who have taken corticosteroids and they did not work well enough.
Jakafi is also used to treat adults and children 12 years of age and older with chronic GVHD who have taken one or two types of treatments and they did not work well enough.
Important Safety Information
Jakafi can cause serious side effects, including:
Low blood counts: Jakafi® (ruxolitinib) may cause low platelet, red blood cell, and white blood cell counts. If you develop bleeding, stop taking Jakafi and call your healthcare provider. Your healthcare provider will do a blood test to check your blood counts before you start Jakafi and regularly during your treatment. Your healthcare provider may change your dose of Jakafi or stop your treatment based on the results of your blood tests. Tell your healthcare provider right away if you develop or have worsening symptoms such as unusual bleeding, bruising, tiredness, shortness of breath, or a fever.
Infection: You may be at risk for developing a serious infection during treatment with Jakafi. Tell your healthcare provider if you develop any of the following symptoms of infection: chills, nausea, vomiting, aches, weakness, fever, painful skin rash or blisters.
Cancer: Some people have had certain types of non-melanoma skin cancers during treatment with Jakafi. Your healthcare provider will regularly check your skin during your treatment with Jakafi. Tell your healthcare provider if you develop any new or changing skin lesions during treatment with Jakafi.
Increases in cholesterol: You may have changes in your blood cholesterol levels during treatment with Jakafi. Your healthcare provider will do blood tests to check your cholesterol levels about every 8 to 12 weeks after you start taking Jakafi, and as needed.
Increased risk of major cardiovascular events such as heart attack, stroke or death in people who have cardiovascular risk factors and who are current or past smokers while using another JAK inhibitor to treat rheumatoid arthritis: Get emergency help right away if you have any symptoms of a heart attack or stroke while taking Jakafi, including: discomfort in the center of your chest that lasts for more than a few minutes, or that goes away and comes back, severe tightness, pain, pressure, or heaviness in your chest, throat, neck, or jaw, pain or discomfort in your arms, back, neck, jaw, or stomach, shortness of breath with or without chest discomfort, breaking out in a cold sweat, nausea or vomiting, feeling lightheaded, weakness in one part or on one side of your body, slurred speech.
Increased risk of blood clots: Blood clots in the veins of your legs (deep vein thrombosis, DVT) or lungs (pulmonary embolism, PE) have happened in people taking another JAK inhibitor for rheumatoid arthritis and may be life-threatening. Tell your healthcare provider right away if you have any signs and symptoms of blood clots during treatment with Jakafi, including: swelling, pain, or tenderness in one or both legs, sudden, unexplained chest or upper back pain, shortness of breath or difficulty breathing.
Possible increased risk of new (secondary) cancers: People who take another JAK inhibitor for rheumatoid arthritis have an increased risk of new (secondary) cancers, including lymphoma and other cancers. People who smoke or who smoked in the past have an added risk of new cancers.
The most common side effects of Jakafi include: for certain types of myelofibrosis (MF) and polycythemia vera (PV) – low platelet or red blood cell counts, bruising, dizziness, headache, and diarrhea; for acute GVHD – low platelet counts, low red or white blood cell counts, infections, and swelling; and for chronic GVHD – low red blood cell or platelet counts and infections including viral infections.
These are not all the possible side effects of Jakafi. Ask your pharmacist or healthcare provider for more information. Call your doctor for medical advice about side effects.
Before taking Jakafi, tell your healthcare provider about: all the medications, vitamins, and herbal supplements you are taking and all your medical conditions, including if you have an infection, have or had low white or red blood cell counts, have or had tuberculosis (TB) or have been in close contact with someone who has TB, had shingles (herpes zoster), have or had hepatitis B, have or had liver or kidney problems, are on dialysis, have high cholesterol or triglycerides, had cancer, are a current or past smoker, had a blood clot, heart attack, other heart problems or stroke, or have any other medical condition. Take Jakafi exactly as your healthcare provider tells you. Do not change your dose or stop taking Jakafi without first talking to your healthcare provider.
Women should not take Jakafi while pregnant or planning to become pregnant. Do not breastfeed during treatment with Jakafi and for 2 weeks after the final dose.
Please see the Full Prescribing Information, which includes a more complete discussion of the risks associated with Jakafi.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch, or call 1-800-FDA-1088.
You may also report side effects to Incyte Medical Information at 1-855-463-3463.
